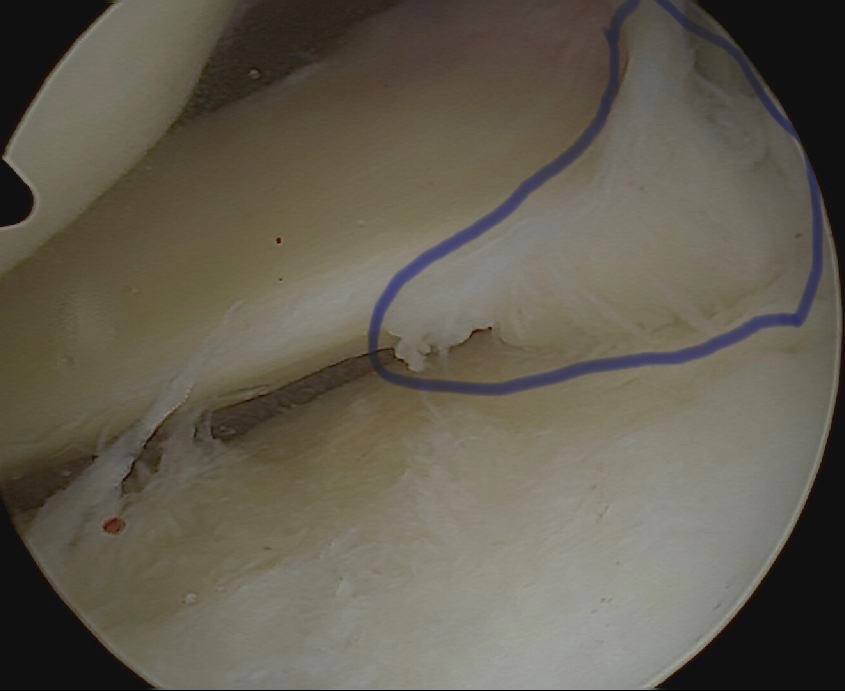
The curious case of the faster-healing knee and the larger steaks
/Some loose ends needed addressing, but why was the recovery so fast?
My doctor took one look at my knee and his jaw dropped. He had hardly ever—or perhaps never—seen a knee that looked that good just four days after arthroscopic surgery.
This clinic specializes in these surgeries, so he sees patients, many of them young athletes, in post-surgical recovery checkups daily. He kept looking at my knee and then looking at me—a middle aged guy. He checked the chart to make sure the surgery was actually just four days ago. Still in disbelief, he asked me what I had done.
What came next was instructive. I told him I thought the surprisingly fast recovery might be due to my very low carb diet.
His response was surreal, because non-existent. He did not acknowledge what I had said. He just kept going on about how good the knee looked and how he had hardly ever seen such a fast recovery.
The rest of the conversation was clear and normal. We talked about how the stitches were coming out next time. We talked about how, given the fast recovery, I probably didn’t need that physical therapy after all.
I was still curious, so I mentioned just once more that maybe the notable recovery could be due to my low-carb diet, because that seems to reduce inflammation.
Once again, no reaction. It was as if I had spoken just that one line in Chinese. No, not even that. Switching to Mandarin would have elicited some noticeable reaction. Would the fact of my statement cease to exist if not acknowledged?
A tale of two otherwise identical surgeries
I have spent several decades in somewhat rough activities including martial arts earlier and amateur adult soccer later. With such activities, it can seem at times like rolling dice when an individual’s luck might run a bit low and an arthroscopic meniscus repair will be called for. Once this kind of tissue tears a little, it just does not heal by itself. Worse, the torn piece can obstruct the joint and lead to additional tearing and other problems. It’s a little like having a hand-knit sweater with a hanging thread that is just waiting to get caught and unravel some more (but with pain involved). The hanging thread just needs to be trimmed off. The invention of arthroscopic technology revolutionized the ease with which this could be done.
My first such surgery was in 2010. Of course, I thought I had learned my lesson and would not be back. But alas, in a single lapse of focus, the other knee over-extended on a bad landing on the futsal court in late 2015, the fault only of myself. So my second such surgery, on the other knee this time, was done recently in 2016.
My recovery six years ago was good, but relatively more ordinary. It at least did not elicit any jaw dropping from the specialist. I recovered nicely, above average, but I do not think I recovered this well.
It was also striking to me after this 2016 surgery that I awakened from anesthesia crisply, with perfect clarity, as if from an unusually excellent night’s sleep. I do not remember a feeling at all like that from my corresponding 2010 recovery room awakening. I recall it as groggy and gradual, more as I would have expected. This may or may not be important or coincidental, but I note that a major effect of a low-carb ketogenic diet is a gradual transformation of preferred cellular fuel sources, including for the brain, so an effect like this is plausible. I have noticed clear improvements in sleep patterns following dietary changes and full anesthesia and sleep are related states.
There is certainly individual variation in recovery rates, but the interesting thing here is the rare opportunity to compare the same person recovering from two identical surgeries at two different times. Six years apart, these were the same surgeries, performed by the same surgeon, and conducted at the same clinic with the same anesthesiologist in the same room. They were for remarkably similar injuries. The surgeries were conducted a similar length of time after the initial incident (in both cases, after about eight months of “conservative” recovery and training efforts). I am the same person. Almost every factor was the same.
So what changed between the two events?
First, I am six years older. But this would predict a slower recovery, not a notably faster one.
Second, I have completely changed my diet, including adding fasting periods. Both low-carb and fasting are known to reduce systemic inflammation compared with more conventional modern diets, with their high frequency, high refined carbs, and brutally high omega six. With lower systemic inflammation (call it immune-system noise), specific inflammation as a healing response at the surgery site (immune-system signal) might proceed with more appropriate focus on the local site and without undue exaggeration.
It was only several months after the 2010 surgery that I discovered The Primal Blueprint and first ditched grains, started even more thoroughly avoiding refined sugars, and replaced industrial processed seed (“vegetable”) oils with natural fats. Then, starting around 2013, I moved toward a still lower-carb, higher-fat whole food ketogenic approach. More recently, just within 2016, and mainly in the past few months, I have been trying out a largely carnivorous approach and have introduced more fasting and intermittent fasting as well.
Analysis and implications
Unfortunately, I have no comparable record of the state of the other knee after exactly four days in 2010, only necessarily unreliable memories and impressions. I could be making this up from memory and confirmation bias. Or the difference between the surgeries could be random or due to some other unnoticed factor.
Still, even as anecdote, these recollections strike me as notable. And on reflection, it occurs to me that one of the sad symptoms of diabetes is poorer wound healing. If a low-carb (and natural fats) diet tends to lead toward the very opposite of a diabetes crisis metabolism, might it not likewise lead to the opposite of compromised wound healing? That is, improved and above-average wound healing. This seems plausible.
The hypothesis here is that conventional high-frequency, high-carb diets might keep most people’s post-operative and other wounds from healing as quickly as they might otherwise. The effects of the resulting unnecessary systemic inflammation would come to appear “normal” only because it would be what clinics would see from day to day within the particular afflicted populations. Anyone doing something quite atypical of that population, such as a very low carb diet, might produce seeming anomalies—relative to this afflicted population. If lower carb and fasting are superior to higher carb and frequent eating, as I have come to think they are—through research, countless biographical and ethnographic reports, and accumulating personal experience—those anomalies would show up as positive surprises.
Greater clarity here could support dietary practices that improve health outcomes while reducing, or at least not adding to, reliance on the medication industry. As I put it in the title of my book review essay on Jason Fung's The Obesity Code, “Only the faster profits.”
Relatively little research money floods in to verify or falsify these types of potential effects, perhaps, because no potentially profitable pills would be entailed in producing them. If such benefits might be real, people changing their own habits would be the primary beneficiaries and direct action to make personal changes would be the primary method.